Key Features & Benefits
Clinically relevant – Recapitulates human pemphigus vulgaris with anti-DSG3 autoantibodies, acantholysis, and skin blistering.
Mechanism-driven – DSG3 immunization induces pathogenic autoantibodies that target desmoglein 3, disrupting keratinocyte adhesion and causing blister formation.
Comprehensive endpoints – Body weight, serum anti-DSG3 antibody titers (ELISA), skin histopathology (HE with acantholysis scoring), clinical observation of skin lesions (hair loss, ulceration).
Translational value – Ideal for testing biologics (rituximab, anti-CD20), immunomodulators (corticosteroids, mycophenolate), and FcRn blockers (efgartigimod).
IND-ready data packages – Studies can be conducted in accordance with GLP principles.
Technical Data & Validation
DSG3 induced Pemphigus Model in C57BL/6 mice
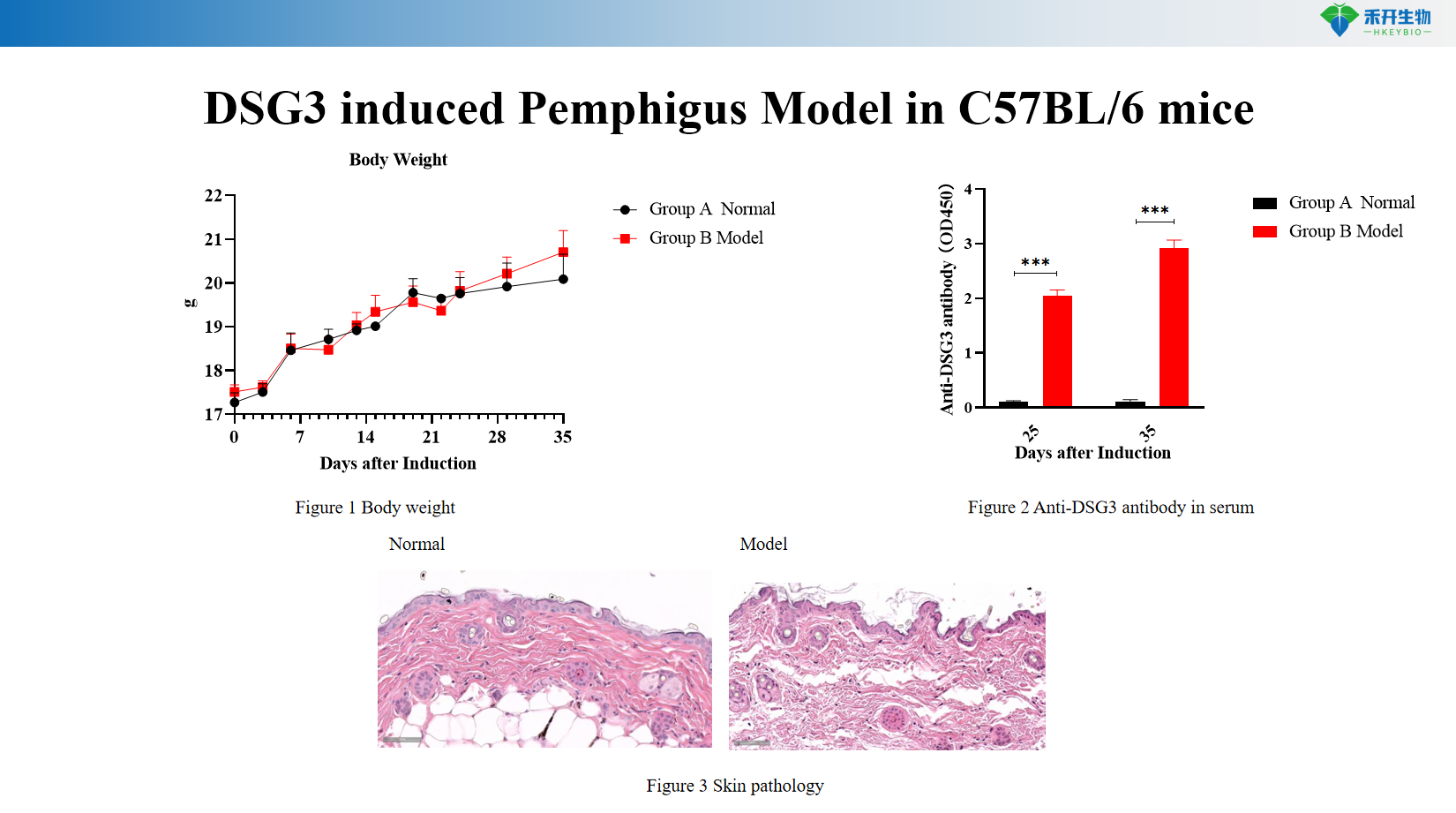
Applications
• Efficacy testing of biologics targeting B cells (rituximab, obinutuzumab) and plasma cells (anti-CD38)
• Evaluation of FcRn blockers (efgartigimod, nipocalimab) and complement inhibitors
• Testing of immunomodulators (corticosteroids, mycophenolate mofetil, azathioprine) and JAK inhibitors
• Target validation for desmoglein-specific autoimmunity and blister formation pathways
• IND-enabling pharmacology and toxicology studies
Model Specifications
Parameter | Specification |
Species/Strain | C57BL/6 mouse |
Induction method | Immunization with desmoglein 3 (DSG3) protein in adjuvant |
Key Features | Body weight changes, elevated serum anti-DSG3 antibodies, epidermal acantholysis, antibody deposition, skin histopathology (HE), localized hair loss, ulceration |
| Data package | Raw data, analysis reports, ELISA results, histology slides, clinical photographs, bioinformatics (optional) |
❓ Frequently Asked Questions
Q: How does DSG3 immunization induce pemphigus?
A: DSG3 is a key autoantigen in pemphigus vulgaris. Immunization with DSG3 protein breaks immune tolerance, leading to production of pathogenic anti-DSG3 antibodies. These antibodies bind to desmoglein 3 on keratinocytes, disrupting desmosomal adhesion and causing acantholysis, blister formation, and skin lesions.
Q: What are the key similarities with human pemphigus vulgaris?
A: The model exhibits anti-DSG3 autoantibodies, epidermal acantholysis, blister formation, and IgG deposition along keratinocyte cell surfaces, closely mirroring human pemphigus vulgaris pathology.
Q: Can this model be used for IND-enabling studies?
A: Yes. Studies can be conducted in accordance with GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different DSG3 isoforms, immunization schedules)?
A: Absolutely. Our scientific team tailors immunization protocols, treatment schedules, and endpoint analyses to your specific drug candidate.
Q: What is the typical timeline for a pilot efficacy study?
A: Pilot studies typically run 6–8 weeks post-immunization, including autoantibody development, disease manifestation, and endpoint analysis.

























