Main features and benefits
Clinically Relevant - Outlines the pulmonary fibrosis, cutaneous fibrosis, and TGF-β-mediated pathology of human SSc-ILD.
Composite endpoint - body weight, skin lift height (cutaneous fibrosis), lung function, flow cytometry (immune cell infiltration), lung histopathology (HE and Masson staining).
Mechanistically driven —BLM induces DNA damage, oxidative stress, and TGF-β pathway activation, reflecting the pathogenesis of human SSc-ILD.
Translational value – ideal for testing antifibrotic drugs (nintedanib, pirfenidone), TGF-β inhibitors and immunomodulators.
IND Ready Packet – Research can be conducted in accordance with GLP principles.
Technical data and verification
BLM-induced C57BL/6 SSc-ILD model
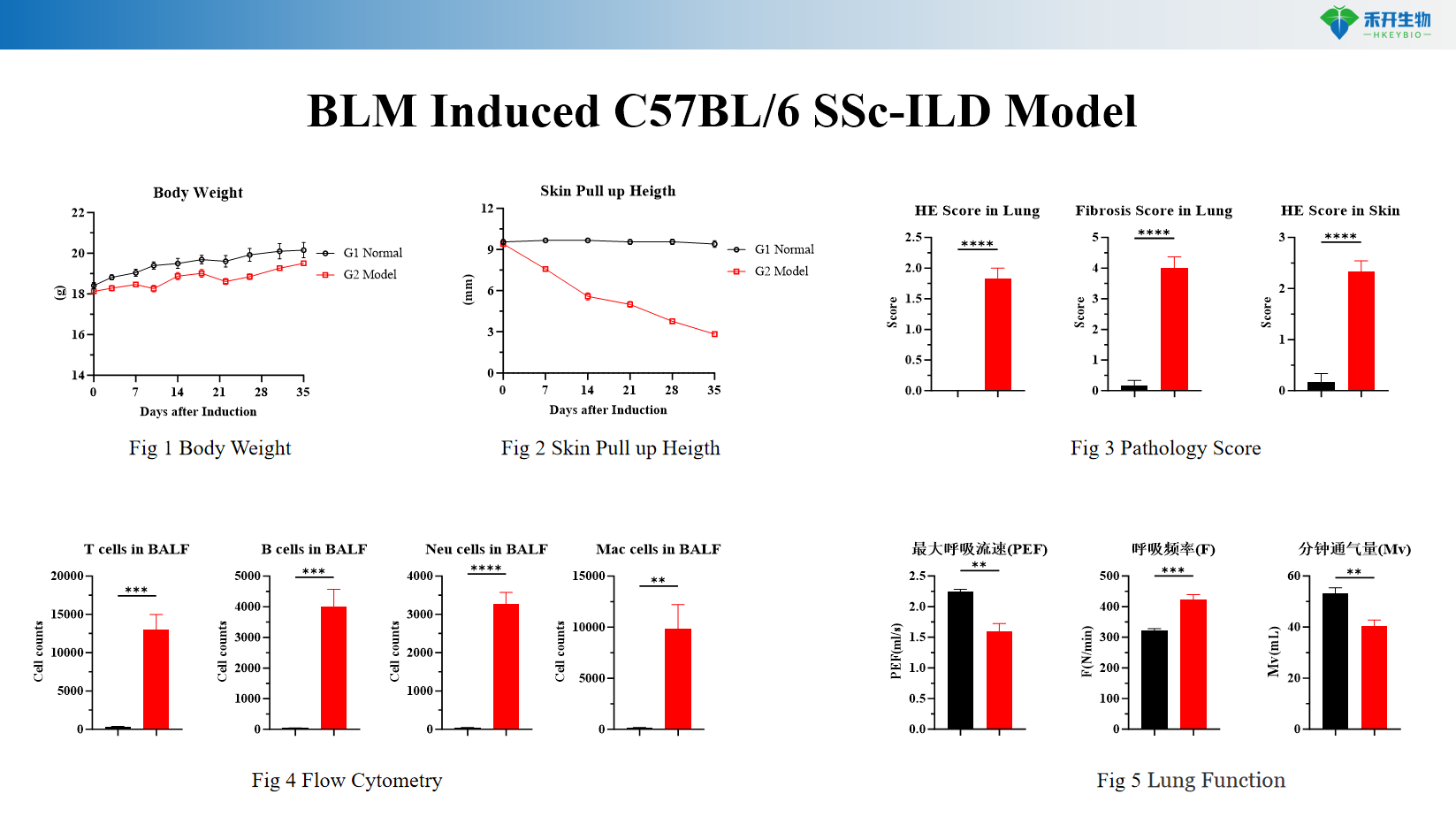
Application areas
• Efficacy testing of antifibrotic drugs (nintedanib, pirfenidone, TGF-β inhibitors, galectin-3 inhibitors)
• Evaluation of immunomodulators targeting inflammation and fibrosis
• Target validation of TGF-β signaling and fibrotic pathways
• Biomarker discovery (collagen markers, inflammatory mediators, immune cell signatures)
• Pharmacology and toxicology studies to support IND
Model specifications
scope | Specification |
Species/Strain | C57BL/6 mouse |
induction method | Intratracheal infusion of bleomycin (BLM, 1-2 U/kg) in normal saline, single dose |
study time | 14–28 days (fibrosis development) |
critical endpoint | Body weight, skin pull-up height (cutaneous fibrosis), lung function (compliance, resistance), flow cytometry (immune cell infiltration: macrophages, neutrophils, T cells), lung histopathology (HE and Masson's trichrome staining and Ashcroft score), optional: hydroxyproline content, BALF cell count, cytokine levels |
| positive control | Nintedanib or pirfenidone may be used as reference antifibrotic compounds |
packet | Raw data, analysis reports, lung function data, flow cytometry files, histology slides (HE, Masson), bioinformatics (optional) |
❓ FAQ
Question: How does bleomycin induce SSc-ILD in mice?
A: Intratracheal bleomycin induces DNA damage and oxidative stress in lung tissue, leading to persistent inflammation, activation of the TGF-β signaling pathway, and excessive extracellular matrix deposition, similar to the cutaneous and pulmonary fibrosis seen in human SSc-ILD.
Q: What are the key similarities to human SSc-ILD?
A: This model exhibits progressive pulmonary fibrosis (HE and Masson staining), decreased lung function, skin fibrosis, and immune cell infiltration, which are closely related to human SSc-ILD pathology.
Q: Can this model be used for IND support studies?
Answer: Yes. Studies can be conducted according to GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different BLM doses, timing of treatment, combination with other drugs)?
Answer: Of course. Our scientific team tailors induction protocols, treatment plans and endpoint analyzes for your specific drug candidate.
Q: What is the typical timeline for a pilot efficacy study?
A: Pilot studies are typically conducted 21-28 days after BLM instillation, fibrosis develops within 14-21 days, and treatment is performed during or after induction.





























