Key Features & Benefits
Clinically relevant – Recapitulates human IIM: muscle weakness, inflammatory infiltration, and elevated pro-inflammatory cytokines (IL-6, IL-17A).
Quantifiable endpoints – Body weight, muscle strength (grip strength test), serum cytokine levels (IL-6, IL-17A), muscle histopathology (HE scoring), inflammatory cell infiltration.
Mechanism-driven – Myosin immunization triggers autoimmune response against skeletal muscle, involving both cellular (Th1/Th17) and humoral immunity, mirroring human myositis pathogenesis.
Translational value – Ideal for testing immunosuppressants (corticosteroids, methotrexate, mycophenolate), biologics targeting IL-6 (tocilizumab), IL-17 (secukinumab), and JAK inhibitors.
IND-ready data packages – Studies can be conducted in accordance with GLP principles.
Technical Data & Validation
Myosin Induced BALB/c DM Model
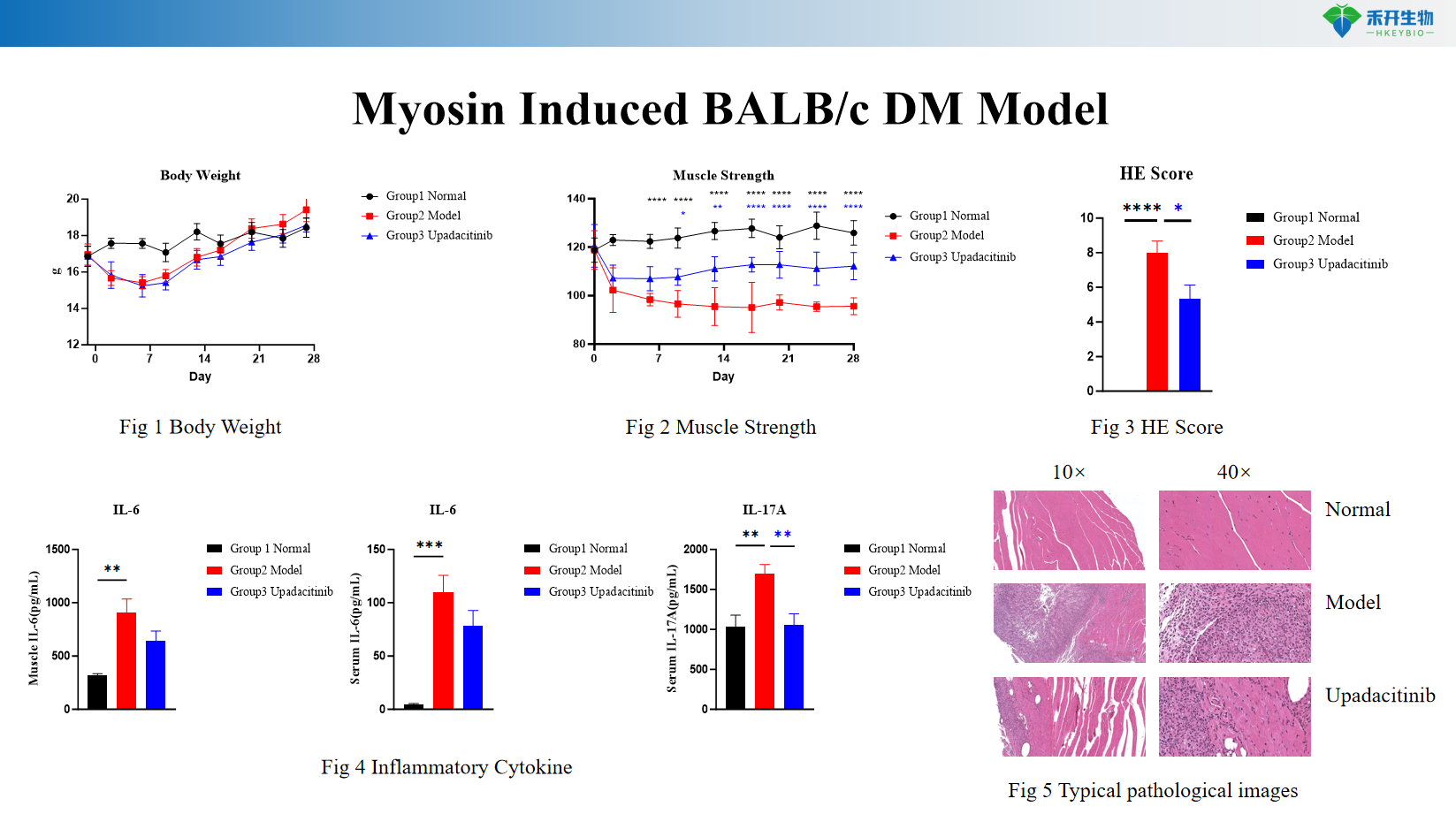
Applications
• Efficacy testing of immunosuppressants (corticosteroids, methotrexate, mycophenolate mofetil, cyclophosphamide)
• Evaluation of biologics targeting IL-6 (tocilizumab), IL-17 (secukinumab, ixekizumab), and JAK inhibitors (tofacitinib, baricitinib)
• Target validation for Th17 and Th1 pathways in autoimmune myositis
• Biomarker discovery (cytokine signatures, autoantibodies, muscle damage markers)
• IND-enabling pharmacology and toxicology studies
Model Specifications
Parameter | Specification |
Species/Strain | BALB/c mouse |
Induction method | Immunization with myosin protein (e.g., rabbit or bovine myosin) emulsified in CFA, with or without booster injections |
Study duration | 4–8 weeks post-immunization (depending on disease progression) |
Key endpoints | Body weight, muscle strength (grip strength test), serum cytokine levels (IL-6, IL-17A), muscle histopathology (HE staining with scoring for inflammation, necrosis, regeneration), optional: flow cytometry of muscle-infiltrating immune cells, anti-myosin autoantibodies |
Data package | Raw data, analysis reports, behavioral data, histology slides, cytokine ELISA results, bioinformatics (optional) |
❓ Frequently Asked Questions
Q: How does myosin immunization induce myositis?
A: Myosin is a major structural protein of skeletal muscle. Immunization with myosin in adjuvant breaks immune tolerance, leading to activation of autoreactive T cells (Th1/Th17) and production of anti-myosin antibodies. These immune effectors infiltrate muscle tissue, causing inflammation, myofiber necrosis, and functional deficits, closely mimicking human idiopathic inflammatory myopathy.
Q: What are the key similarities with human IIM?
A: The model exhibits muscle weakness, weight loss, inflammatory cell infiltration in muscle, elevated pro-inflammatory cytokines (IL-6, IL-17A), and histopathological changes (necrosis, regeneration) mirroring human polymyositis/dermatomyositis.
Q: Can this model be used for IND-enabling studies?
A: Yes. Studies can be conducted in accordance with GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different myosin sources, adjuvants, treatment schedules)?
A: Absolutely. Our scientific team tailors immunization protocols, treatment schedules, and endpoint analyses to your specific drug candidate.
Q: What is the typical timeline for a pilot efficacy study?
A: Pilot studies are typically completed within 6–8 weeks, including immunization, disease development, and endpoint analysis.















