Key Features & Benefits
Clinically relevant – Ischemia-reperfusion injury is a major cause of human AKI, mimicking clinical scenarios such as shock, surgery, or transplantation.
Comprehensive endpoints – Serum creatinine (CREA-S), albuminuria (ALB), renal histopathology (HE staining) with scoring for tubular injury, cast formation, and inflammation.
Mechanism-driven – Recapitulates key pathophysiological processes: hypoxia, oxidative stress, inflammation, and tubular cell death.
Translational value – Ideal for testing renoprotective agents, antioxidants, anti-inflammatory drugs, and cell-based therapies.
IND-ready data packages – Studies can be conducted in accordance with GLP principles.
Technical Data & Validation
Ischemia-reperfusion Induced Acute Kidney Injury Model
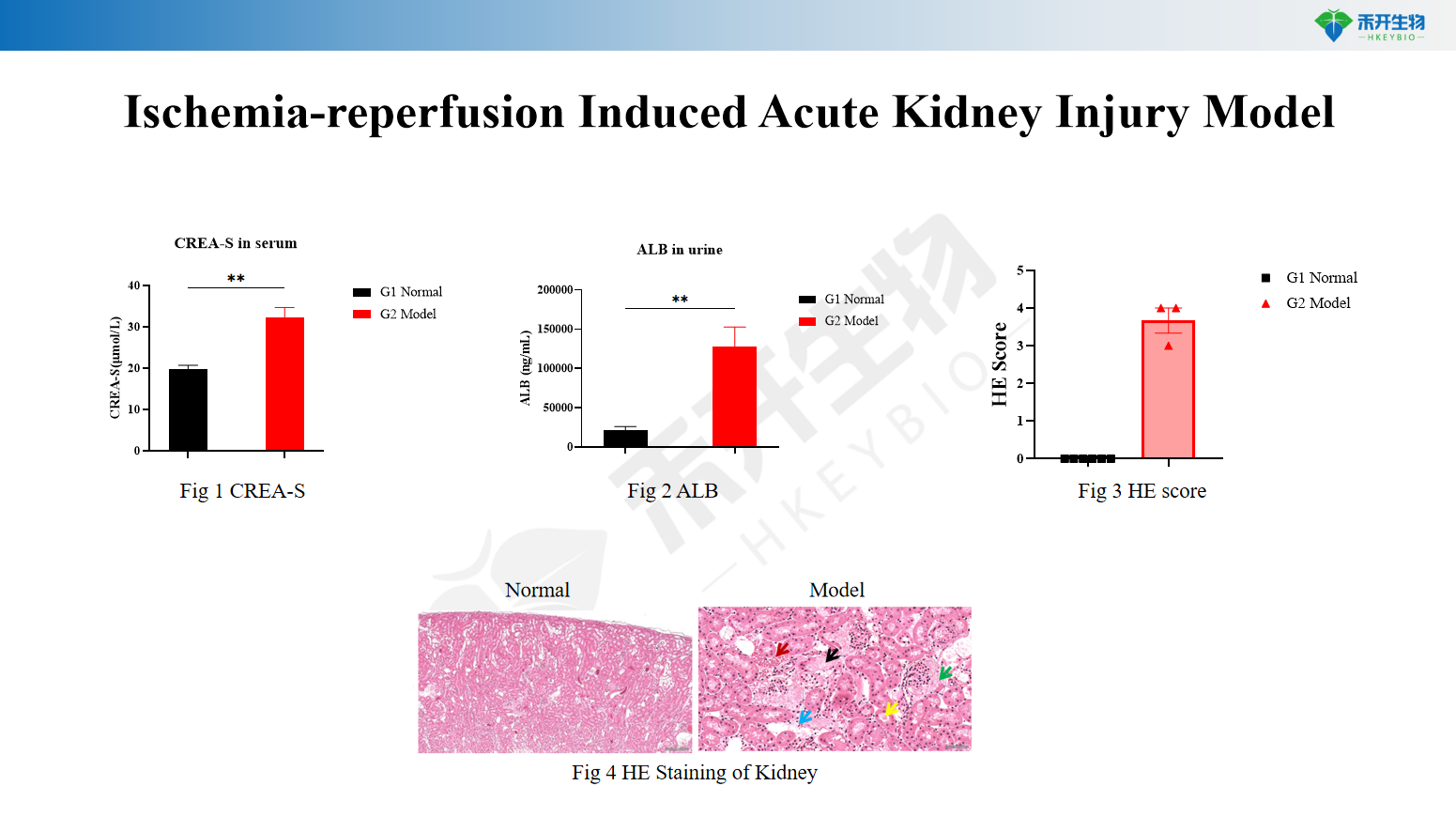
Applications
• Efficacy testing of renoprotective agents (antioxidants, vasodilators, anti-inflammatory drugs)
• Evaluation of cell-based therapies (MSCs, extracellular vesicles) and regenerative medicine approaches
• Target validation for ischemic injury pathways (hypoxia-inducible factors, oxidative stress, inflammation)
• Biomarker discovery (early kidney injury markers, inflammatory mediators)
• IND-enabling pharmacology and toxicology studies
Model Specifications
Parameter | Specification |
Species/Strain | C57BL/6 mouse |
Induction method | Bilateral renal pedicle clamping (20–45 min) under anesthesia, followed by reperfusion (24–72 hours) |
Study duration | Acute: 24–72 hours; subacute/chronic: up to 14 days (for AKI-to-CKD transition studies) |
Key endpoints | Serum creatinine (CREA-S), albuminuria (ALB), renal histopathology (HE staining with tubular injury score), optional: BUN, KIM-1, NGAL, oxidative stress markers (MDA, SOD), inflammatory cytokines (IL-6, TNF-α, MCP-1), TUNEL apoptosis assay |
Data package | Raw data, analysis reports, clinical chemistry, histology slides (HE), bioinformatics (optional) |
❓ Frequently Asked Questions
Q: How does ischemia-reperfusion induce AKI in mice?
A: Temporary clamping of the renal pedicle interrupts blood flow, causing ischemic injury to tubular epithelial cells. Upon clamp release, reperfusion triggers oxidative stress, inflammation, and additional cellular damage, culminating in acute kidney injury.
Q: What are the key similarities with human AKI?
A: The model exhibits elevated serum creatinine, albuminuria, tubular necrosis, cast formation, and inflammation, closely resembling human ischemic AKI seen in shock, surgery, or transplantation settings.
Q: Can this model be used for IND-enabling studies?
A: Yes. Studies can be conducted in accordance with GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different ischemia times, unilateral vs. bilateral clamping)?
A: Absolutely. Our scientific team tailors ischemia duration, clamping method (unilateral or bilateral), reperfusion time points, and endpoint analyses to your specific drug candidate.




























