Key Features & Benefits
Multiple susceptible strains – C57BL/6, DBA/1 mice and Wistar rats available to suit different genetic backgrounds and experimental needs.
Clinically relevant – Recapitulates human anti-GBM disease with acute crescentic glomerulonephritis, renal dysfunction, and characteristic histopathology.
Comprehensive endpoints – Body weight, serum CREA-S, proteinuria, UACR, renal histopathology (HE scoring and crescent quantification).
Mechanism-driven – Direct antibody-mediated injury to glomerular basement membrane triggers complement activation and inflammatory cascade.
Translational value – Ideal for testing immunosuppressants (cyclophosphamide, glucocorticoids), biologics (rituximab, anti-CD20), complement inhibitors, and plasma exchange mimetics.
IND-ready data packages – Studies can be conducted in accordance with GLP principles.
Technical Data & Validation
Anti-GBM Induced GBM Model
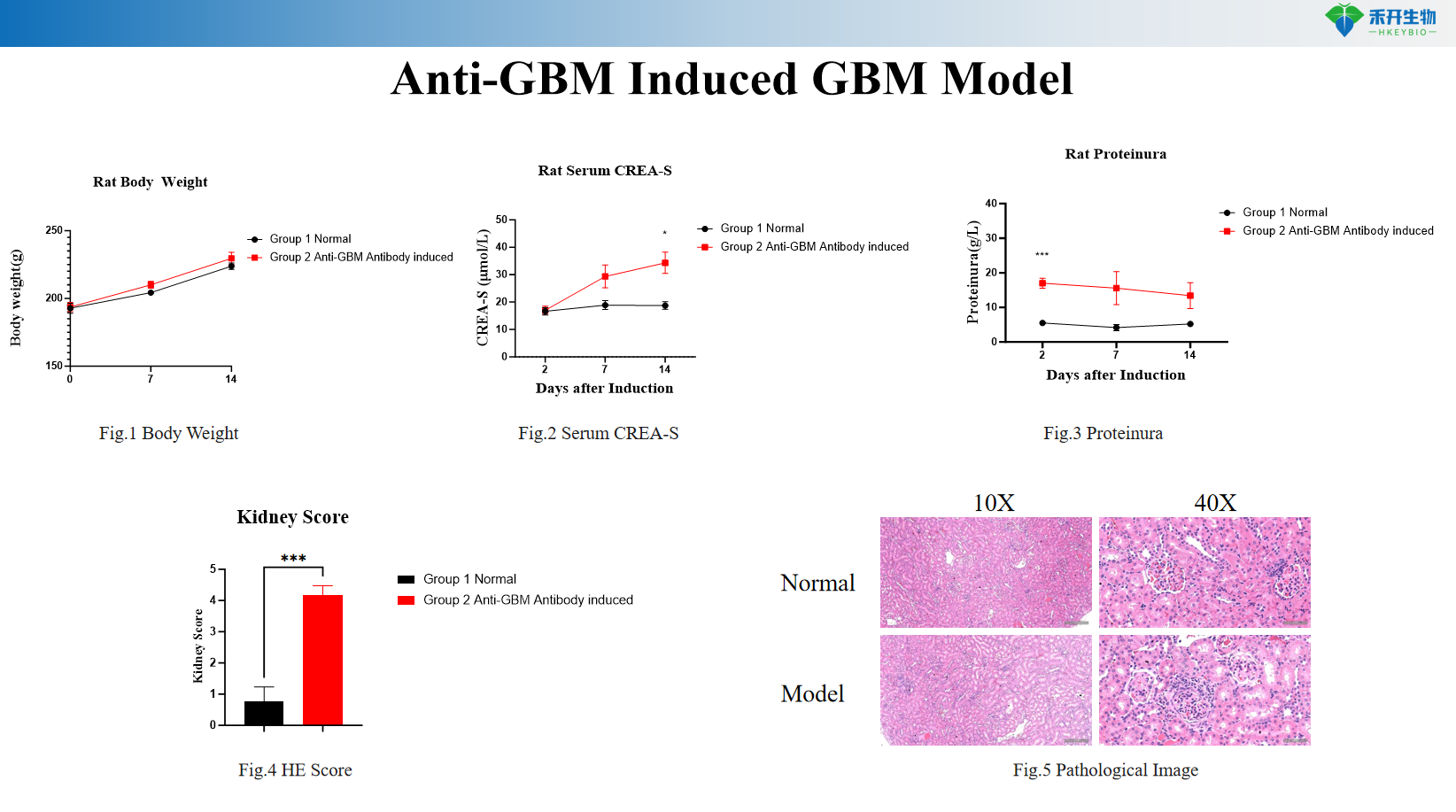
Applications
• Efficacy testing of immunosuppressants (cyclophosphamide, glucocorticoids, mycophenolate)
• Evaluation of biologics (rituximab, anti-CD20, anti-CD19) and plasma exchange mimetics
• Testing of complement inhibitors (anti-C5, C5aR antagonists)
• Target validation for antibody-mediated glomerulonephritis
• IND-enabling pharmacology and toxicology studies
Model Specifications
Parameter | Specification |
Species/Strain | Sprague-Dawley (SD) rat |
Induction method | Intravenous injection of heterologous anti-GBM serum (nephrotoxic serum) |
Study duration | 7–21 days (acute phase) |
Key endpoints | Body weight, serum creatinine (CREA-S), proteinuria, urinary albumin-to-creatinine ratio (UACR), blood urea nitrogen (BUN), renal histopathology (HE staining with crescent scoring, glomerulonephritis assessment), optional: complement deposition (C3 immunofluorescence), lung histopathology for alveolar hemorrhage |
Data package | Raw data, analysis reports, clinical chemistry, urine analysis, histology slides, bioinformatics (optional) |
❓ Frequently Asked Questions
Q: How does anti-GBM serum induce glomerulonephritis?
A: Heterologous anti-GBM antibodies bind to the glomerular basement membrane, activating complement and recruiting inflammatory cells. This triggers crescent formation, glomerular injury, and rapid decline in renal function, mimicking human anti-GBM disease.
Q: What are the key similarities with human anti-GBM disease?
A: The model exhibits acute crescentic glomerulonephritis, proteinuria, elevated serum creatinine, and characteristic linear immunoglobulin deposition along the GBM, closely resembling human Goodpasture syndrome.
Q: Can this model be used for IND-enabling studies?
A: Yes. Studies can be conducted in accordance with GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different anti-GBM serum doses, timing of intervention)?
A: Absolutely. Our scientific team tailors induction protocols, treatment schedules, and endpoint analyses to your specific drug candidate.































