Key Features & Benefits
Clinically relevant – Recapitulates human SSc-ILD with pulmonary fibrosis, skin fibrosis, and TGF-β mediated pathology.
Comprehensive endpoints – Body weight, skin pull-up height (skin fibrosis), lung function, flow cytometry (immune cell infiltration), lung histopathology (HE & Masson staining).
Mechanism-driven – BLM induces DNA damage, oxidative stress, and TGF-β pathway activation, mirroring human SSc-ILD pathogenesis.
Translational value – Ideal for testing anti-fibrotic agents (nintedanib, pirfenidone), TGF-β inhibitors, and immunomodulators.
IND-ready data packages – Studies can be conducted in accordance with GLP principles.
Technical Data & Validation
BLM Induced C57BL/6 SSc-ILD Model
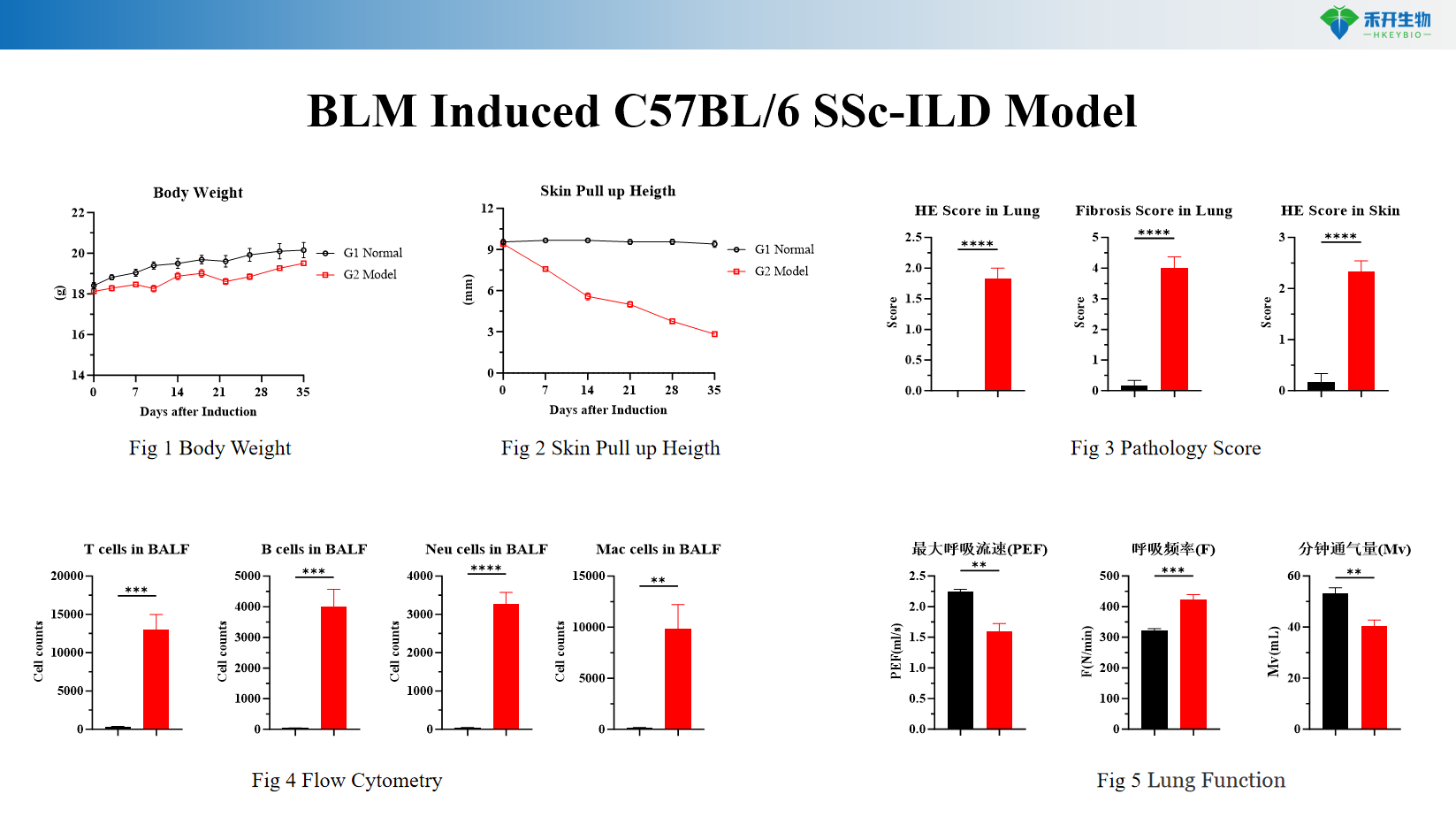
Applications
• Efficacy testing of anti-fibrotic agents (nintedanib, pirfenidone, TGF-β inhibitors, galectin-3 inhibitors)
• Evaluation of immunomodulators targeting inflammation and fibrosis
• Target validation for TGF-β signaling and fibrotic pathways
• Biomarker discovery (collagen markers, inflammatory mediators, immune cell signatures)
• IND-enabling pharmacology and toxicology studies
Model Specifications
Parameter | Specification |
Species/Strain | C57BL/6 mouse |
Induction method | Intratracheal instillation of bleomycin (BLM, 1–2 U/kg) in saline, single dose |
Study duration | 14–28 days (fibrosis development) |
Key endpoints | Body weight, skin pull-up height (skin fibrosis), lung function (compliance, resistance), flow cytometry (immune cell infiltration: macrophages, neutrophils, T cells), lung histopathology (HE and Masson trichrome staining with Ashcroft score), optional: hydroxyproline content, BALF cell counts, cytokine levels |
| Positive control | Nintedanib or pirfenidone available as reference anti-fibrotic compounds |
Data package | Raw data, analysis reports, lung function data, flow cytometry files, histology slides (HE, Masson), bioinformatics (optional) |
❓ Frequently Asked Questions
Q: How does bleomycin induce SSc-ILD in mice?
A: Intratracheal bleomycin triggers DNA damage and oxidative stress in lung tissue, leading to persistent inflammation, activation of the TGF-β signaling pathway, and excessive extracellular matrix deposition, mimicking both skin and lung fibrosis seen in human SSc-ILD.
Q: What are the key similarities with human SSc-ILD?
A: The model exhibits progressive pulmonary fibrosis (HE and Masson staining), lung function decline, skin fibrosis, and immune cell infiltration, closely mirroring human SSc-ILD pathology.
Q: Can this model be used for IND-enabling studies?
A: Yes. Studies can be conducted in accordance with GLP principles for regulatory submissions (FDA, EMA).
Q: Do you offer customized study protocols (e.g., different BLM doses, treatment timing, combination with other agents)?
A: Absolutely. Our scientific team tailors induction protocols, treatment schedules, and endpoint analyses to your specific drug candidate.
Q: What is the typical timeline for a pilot efficacy study?
A: Pilot studies typically run 21–28 days post-BLM instillation, with fibrosis developing over 14–21 days and treatment administered during or after induction.





























